Our website is made possible by displaying online advertisements to our visitors.
Please consider supporting us by disabling your ad blocker.
Clostridioides difficile
| Clostridioides difficile | |
|---|---|

| |
| C. difficile colonies on a blood agar plate | |
| |
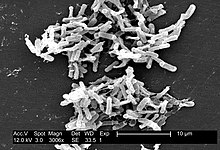
| Electron micrograph of the bacterium | |
| Scientific classification | |
| Domain: | Bacteria |
| Phylum: | Bacillota |
| Class: | Clostridia |
| Order: | Eubacteriales |
| Family: | Peptostreptococcaceae |
| Genus: | Clostridioides |
| Species: | C. difficile
|
| Binomial name | |
| Clostridioides difficile (Hall & O'Toole, 1935) Lawson & Rainey, 2016
| |
| Synonyms | |
Clostridioides difficile (syn. Clostridium difficile) is a bacterium known for causing serious diarrheal infections, and may also cause colon cancer.[4][5] It is known also as C. difficile, or C. diff (/siː dɪf/), and is a Gram-positive species of spore-forming bacteria.[6] Clostridioides spp. are anaerobic, motile bacteria, ubiquitous in nature and especially prevalent in soil. Its vegetative cells are rod-shaped, pleomorphic, and occur in pairs or short chains. Under the microscope, they appear as long, irregular (often drumstick- or spindle-shaped) cells with a bulge at their terminal ends (forms subterminal spores). Under Gram staining, C. difficile cells are Gram-positive and show optimum growth on blood agar at human body temperatures in the absence of oxygen. C. difficile is catalase- and superoxide dismutase-negative, and produces up to three types of toxins: enterotoxin A, cytotoxin B and Clostridioides difficile transferase.[7] Under stress conditions, the bacteria produce spores that are able to tolerate extreme conditions that the active bacteria cannot tolerate.[8]
Clostridioides difficile is an important emerging human pathogen; according to the CDC, in 2017 there were 223,900 cases in hospitalized patients and 12,800 deaths in the United States.[9] Although C. difficile is commonly known as a hospital and antibiotic associated pathogen, at most one third of infections can be traced to transmission from an infected person in hospitals,[10] and only a small number of antibiotics are directly associated with an elevated risk of developing a C. difficile infection (CDI), namely vancomycin, clindamycin, fluoroquinolones and cephalosporins.[11][12][13] The majority of infections are acquired outside of hospitals, and most antibiotics have similar elevated risk of infection on par with many non-antibiotic risk factors, such as using stool softeners and receiving an enema.[14]
Clostridioides difficile can also become established in the human colon without causing disease.[15] Although early estimates indicated that C. difficile was present in 2–5% of the adult population,[8] more recent research indicates colonization is closely associated with a history of unrelated diarrheal illnesses, such as food poisoning or laxative abuse.[16] Individuals with no history of gastrointestinal disturbances appear unlikely to become asymptomatic carriers. These carriers are thought to be a major reservoir of infection.[17]
- ^ Cite error: The named reference
Hall et al., 1935was invoked but never defined (see the help page). - ^ Cite error: The named reference
Prevot, 1938was invoked but never defined (see the help page). - ^ Page Species: Clostridioides difficile on "LPSN - List of Prokaryotic names with Standing in Nomenclature". Deutsche Sammlung von Mikroorganismen und Zellkulturen. Archived from the original on November 8, 2022. Retrieved November 8, 2022.
- ^ Drewes JL, Chen J, Markham NO, Knippel RJ, Domingue JC, Tam AJ, et al. (August 2022). "Human Colon Cancer-Derived Clostridioides difficile Strains Drive Colonic Tumorigenesis in Mice". Cancer Discovery. 12 (8): 1873–1885. doi:10.1158/2159-8290.CD-21-1273. PMC 9357196. PMID 35678528.
- ^ "Johns Hopkins Doctors Discover That a Common Infection May Cause Cancer". August 24, 2022. Archived from the original on May 26, 2023. Retrieved August 29, 2022.
- ^ Moreno MA, Furtner F, Rivara FP (June 2013). "Clostridium difficile: a cause of diarrhea in children". JAMA Pediatrics. 167 (6): 592. doi:10.1001/jamapediatrics.2013.2551. PMID 23733223.
- ^ Kordus SL, Thomas AK, Lacy DB (May 2022). "Clostridioides difficile toxins: mechanisms of action and antitoxin therapeutics". Nature Reviews. Microbiology. 20 (5): 285–298. doi:10.1038/s41579-021-00660-2. PMC 9018519. PMID 34837014.
- ^ a b Ryan KJ, Ray CG, eds. (2004). Sherris Medical Microbiology (4th ed.). McGraw Hill. pp. 322–4. ISBN 978-0-8385-8529-0.
- ^ "Clostridioides difficile Infection | HAI | CDC". www.cdc.gov. January 2, 2020. Archived from the original on March 8, 2020. Retrieved March 10, 2020.
- ^ Eyre DW, Cule ML, Wilson DJ, Griffiths D, Vaughan A, O'Connor L, et al. (September 2013). "Diverse sources of C. difficile infection identified on whole-genome sequencing". The New England Journal of Medicine. 369 (13): 1195–1205. doi:10.1056/NEJMoa1216064. PMC 3868928. PMID 24066741.
- ^ Guh AY, Adkins SH, Li Q, Bulens SN, Farley MM, Smith Z, et al. (October 1, 2017). "Risk Factors for Community-Associated Clostridium difficile Infection in Adults: A Case-Control Study". Open Forum Infectious Diseases. 4 (4): ofx171. doi:10.1093/ofid/ofx171. PMC 5903408. PMID 29732377.
- ^ Brown KA, Khanafer N, Daneman N, Fisman DN (May 2013). "Meta-analysis of antibiotics and the risk of community-associated Clostridium difficile infection". Antimicrobial Agents and Chemotherapy. 57 (5): 2326–2332. doi:10.1128/AAC.02176-12. PMC 3632900. PMID 23478961.
- ^ Rafey A, Jahan S, Farooq U, Akhtar F, Irshad M, Nizamuddin S, et al. (May 2023). "Antibiotics Associated With Clostridium difficile Infection". Cureus. 15 (5): e39029. doi:10.7759/cureus.39029. PMC 10266117. PMID 37323360.
- ^ McFarland LV, Surawicz CM, Stamm WE (September 1990). "Risk factors for Clostridium difficile carriage and C. difficile-associated diarrhea in a cohort of hospitalized patients". The Journal of Infectious Diseases. 162 (3): 678–684. doi:10.1093/infdis/162.3.678. PMID 2387993.
- ^ McFarland LV, Mulligan ME, Kwok RY, Stamm WE (January 1989). "Nosocomial acquisition of Clostridium difficile infection". The New England Journal of Medicine. 320 (4): 204–210. doi:10.1056/NEJM198901263200402. PMID 2911306.
- ^ VanInsberghe D, Elsherbini JA, Varian B, Poutahidis T, Erdman S, Polz MF (April 2020). "Diarrhoeal events can trigger long-term Clostridium difficile colonization with recurrent blooms". Nature Microbiology. 5 (4): 642–650. doi:10.1038/s41564-020-0668-2. PMID 32042128. S2CID 211074075.
- ^ Eyre DW, Griffiths D, Vaughan A, Golubchik T, Acharya M, O'Connor L, et al. (November 12, 2013). Chang YF (ed.). "Asymptomatic Clostridium difficile colonisation and onward transmission". PLOS ONE. 8 (11): e78445. Bibcode:2013PLoSO...878445E. doi:10.1371/journal.pone.0078445. PMC 3827041. PMID 24265690.
Previous Page Next Page
مطثيه عسيره ARZ Clostridioides difficile Catalan Clostridioides difficile Czech Clostridioides difficile German Clostridioides difficile Spanish Clostridioides difficile French Clostridioides difficile GA Clostridioides difficile HE Clostridioides difficile Hungarian Clostridioides difficile Italian


